7. Feelings of hopelessness

This is a common symptom in major depression and bipolar disorder, and makes patients more susceptible and dangerous when present because it is associated with a higher risk of suicide and suicidal thoughts. Since these patients are not likely to speak up and chat about their feelings, it is often undetected until suicidal behaviour starts.
Thus, if you feel a family member or your loved one is having a different attitude towards life and may need professional help, talk to your doctor about your concern and follow his recommendations. It is important to evaluate and treat every case individually, and early diagnosis and treatment will always bear the best outcomes.
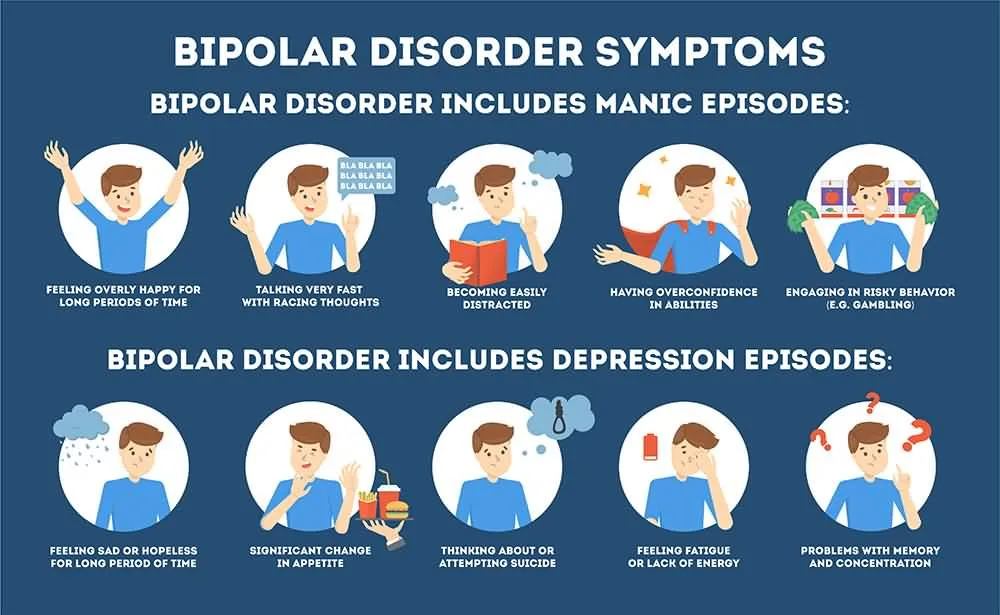
Patients with bipolar disorder may or may not cycle in and out of maniac and depressive episodes. They may stay in between them and live a normal life for a while and then experience a setback once again. Psychotherapy along with medication is one of the best treatments to improve the symptoms in these patients, and the goal is to force the patient out of their maniac or depressive episode with medication to treat them afterwards and maintain them in a state that is in-between both extreme episodic symptoms.
Many of the symptoms described above are found in patients with major depression. Others are shared with patients with schizophrenia and other psychotic alterations. Therefore, it is important to talk to your doctor if this list of signs and symptoms rang any bell or warning signal. Mild cases of bipolar disorder are easier to treat, but they may be more difficult to detect and may go unnoticed. Thus, do not neglect your symptoms and look for professional help if you suspect anything is wrong with your own behaviour or that of your family members and loved ones.
References
Machado-Vieira, R., Luckenbaugh, D. A., Ballard, E. D., Henter, I. D., Tohen, M., Suppes, T., & Zarate Jr, C. A. (2016). Increased activity or energy as a primary criterion for the diagnosis of bipolar mania in DSM-5: findings from the STEP-BD study. American Journal of Psychiatry, 174(1), 70-76.
Tso, I. F., Grove, T. B., & Taylor, S. F. (2014). Differential hedonic experience and behavioural activation in schizophrenia and bipolar disorder. Psychiatry research, 219(3), 470-476.
Marvel, C. L., & Paradiso, S. (2004). Cognitive and neurological impairment in mood disorders. Psychiatric Clinics, 27(1), 19-36.
Muneer, A. (2014). Catatonia in a patient with bipolar disorder type I. Journal of neurosciences in rural practice, 5(3), 314.
Acosta, F. J., Vega, D., Torralba, L., Navarro, S., Ramallo-Fariña, Y., Fiuza, D., … & Siris, S. G. (2012). Hopelessness and suicidal risk in bipolar disorder. A study in clinically nonsyndromal patients. Comprehensive Psychiatry, 53(8), 1103-1109.


